Is My Child Just Naughty or Is It ADHD? A Paediatrician’s Guide for Indian Parents
Worried about your child’s focus or energy levels? Learn the difference between an active child and ADHD. A paediatrician explains symptoms, diagnosis, and when to seek help in India.
12/13/20255 min read


Is your child always "on the go," like they are driven by a motor?
Do you find yourself repeating the same instruction ten times, only to be ignored?
Are teacher complaints about "careless mistakes" or "disturbing the class" becoming a monthly ritual?
If you found yourself nodding yes, take a deep breath. You are not alone.
In paediatric clinics across India, one of the most common worries parents share is: "Doctor, my child just won't sit still. Is this normal active behaviour, or is it ADHD?"
It is natural to feel anxious when you see terms like Attention Deficit Hyperactivity Disorder (ADHD) online. But before you panic, let’s break this down calmly. Not every energetic child has ADHD, and having ADHD does not mean your child cannot be successful and happy.
Here is what every Indian parent needs to know about ADHD—separated from the myths and fear-mongering.
What Exactly is ADHD?
ADHD is a neurodevelopmental condition—meaning it’s related to how the brain grows and works. It affects the parts of the brain that control attention, impulses, and self-regulation.
Think of the brain like a busy traffic junction. In most children, there is a "traffic policeman" (the brain's executive function) that tells them when to stop, when to go, and which car to focus on. In children with ADHD, this traffic policeman is a bit sleepy or absent. This makes it hard for them to:
Filter out distractions (like a fan whirring or a dog barking outside).
Hit the "brake" on their impulses (speaking before thinking).
Sit still when their body wants to move.
It is not caused by "bad parenting," too much sugar, or laziness. It is a biological difference.
The 3 Main Types of ADHD
You might have a mental image of a boy running wild in a classroom. But ADHD looks different in every child. According to guidelines from the Indian Academy of Pediatrics (IAP), there are three presentations:
1. Predominantly Inattentive (Formerly called ADD)
These children are not hyperactive. In fact, they might be "daydreamers."
Signs: Easily distracted, forgets daily chores (like packing their school bag), struggles to follow multi-step instructions, loses pencils/erasers constantly.
Common Parent Thought: "He is so smart but just lazy." (Note: They aren't lazy; their brain is struggling to focus).
2. Predominantly Hyperactive-Impulsive
These children struggle to sit still and wait.
Signs: Fidgets constantly, talks non-stop, interrupts others, has trouble waiting for their turn in games, runs or climbs in unsafe places.
Common Parent Thought: "She has ants in her pants!"
3. Combined Type
The most common form, where a child shows a mix of both inattention and hyperactivity.
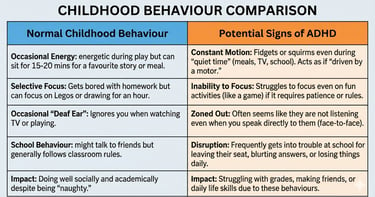
"Is This Normal?" – The Active Child vs. ADHD
This is the trickiest part. All toddlers are impulsive. All primary schoolers get bored. So, how do you tell the difference?
Doctor’s Note: The key difference is impairment. ADHD symptoms affect a child’s life in more than one setting (e.g., both at home AND at school) and persist for more than 6 months.
4 Common Myths Indian Parents Believe (Busted!)
Myth 1: "He can focus on video games for hours, so he can't have ADHD."
Fact: This is called hyperfocus. ADHD brains are drawn to high-stimulation activities (like screens). The struggle is regulating focus on boring or routine tasks, not just paying attention in general.
Myth 2: "ADHD is just a western concept; Indian kids are just pampered."
Fact: ADHD is a global medical condition found in children across all cultures. Research in India shows a prevalence of around 2% to 11% in school-aged children. It is biology, not culture.
Myth 3: "They will outgrow it."
Fact: While hyperactivity often decreases as children become teenagers, inattention usually persists. Without support, "waiting it out" can lead to poor self-esteem, academic failure, and anxiety in teenage years.
Myth 4: "Medicine is the only way and it will drug my child."
Fact: Medication is not the first step for everyone. For young children (under 6), behavioural therapy is the first line of treatment. For older children, medication is safe and highly effective, but it is always part of a larger plan including therapy and lifestyle changes.
Red Flags: When to See a Doctor?
You should consult a Paediatrician or a Developmental Paediatrician if:
Safety is an issue: Your child is impulsive to the point of danger (running into traffic, jumping from heights) despite repeated warnings.
School is a struggle: Teachers constantly report that your child cannot sit still or is falling behind despite being intelligent.
Social isolation: Your child is labeled "aggressive" or "annoying" by peers because they can't wait their turn or respect personal space.
Home life is a battle: Every morning routine or homework session ends in tears and shouting.
What You Can Do at Home (Starting Today)
While waiting for an appointment, try these "brain-friendly" strategies. These help all children, not just those with ADHD.
1. The "One Thing" Rule
Don't say: "Go to your room, put away your bag, wash your hands, and come for lunch." (Too much info!)
Do say: "Please put away your bag." (Wait for it to be done). "Now, go wash your hands."
2. Visual Routines
Children with ADHD struggle with "time blindness." They don't feel time passing.
Use a visual timetable (pictures of brushing teeth, bathing, breakfast).
Use a sand timer or a visual clock for homework (e.g., "Focus for 15 mins, then 5 mins break").
3. Catch Them Being Good
These children hear "No," "Stop," and "Don't" all day. Their self-esteem takes a hit.
Praise the effort: "I saw how hard you tried to sit still during dinner. Well done!"
3:1 Ratio: Try to give 3 positive comments for every 1 correction.
4. Burn the Energy
Exercise increases dopamine—the exact chemical the ADHD brain is low on. Ensure 60 minutes of vigorous play (running, swimming, cycling) every day. Green time (nature) is better than screen time.
Frequently Asked Questions (FAQs)
Q: Can a high-sugar diet cause ADHD?
A: No. While excessive sugar isn't healthy and can cause short-term energy spikes, it does not cause ADHD. However, a balanced diet rich in protein and Omega-3s is great for brain health.
Q: Is ADHD curable?
A: It is a manageable condition, not a disease to be "cured." With the right support (therapy, school accommodations, and sometimes medication), children with ADHD can thrive and often become incredibly creative and successful adults.
Q: Will my child have to take medicine forever?
A: Not necessarily. Medication decisions are reviewed regularly by your doctor. Many children learn coping skills as they grow and may stop medication later, while others find it helpful into adulthood. It is a personal medical choice.
Q: How is ADHD diagnosed in India?
A: There is no single blood test. Diagnosis involves a detailed history from parents, reports from school teachers, and standardized evaluation scales (like the Conners' scale) administered by a paediatrician or psychologist.
A Note from Ybaby
Hearing that your child might have ADHD can feel overwhelming. You might feel protective, scared, or even guilty. Please know this: ADHD is not a label of failure. It is simply a roadmap to understanding how your child’s beautiful, fast-paced brain works.
Early intervention changes everything. If you are concerned, trust your gut and speak to your paediatrician. You aren't looking for a problem; you are looking for a solution to help your child shine.
Does your child struggle with homework battles? Would you like me to give you a simple, printable "After-School Checklist" template designed specifically for distractible kids? DM us here we will send it directly.